|
Case Report
Giant fronto-ethmoido-orbital mucocele. Multidisciplinary management about a case at Saint Joseph Hospital in Kinshasa, Democratic Republic of the Congo
1 ENT Department, Saint Joseph Hospital, Kinshasa, DRC
2 Department of Ophthalmology, Saint Joseph Hospital, Kinshasa, DRC
3 Notre-Dame Tshumbe University, Tshumbe, DRC
4 Department of Ophthalmology, University of Lubumbashi, Lubumbashi, DRC
5 Department of Ophthalmology, Rostock University Medical Center, Rostock, Germany
Address correspondence to:
Omadjela Oluku Augustin
Saint Joseph Hospital, Kinshasa,
DRC
Message to Corresponding Author
Article ID: 100014Z18OA2024
Access full text article on other devices

Access PDF of article on other devices

How to cite this article
Augustin OA, Janvier KN, Damien LM, Asani Y, Noel AN, Rose G, Friedrich GR. Giant fronto-ethmoido-orbital mucocele. Multidisciplinary management about a case at Saint Joseph Hospital in Kinshasa, Democratic Republic of the Congo. J Case Rep Images Otolaryngol 2024;5(2):7–11.ABSTRACT
Introduction: Sinus mucocele is a benign cystic tumor which evolves slowly and may be responsible for ophthalmological and endocranial complications. In this context, its management may require multidisciplinary expertise, which may be lacking in an environment with limited resources.
Case Report: We report the case of a 38-year-old female patient with an ocular globe protuberance and redness of the right eye that had been evolving for several years without consulting specialized services. In the ENT and Ophthalmology Departments, the clinical signs were dominated by axile exophthalmos and visual impairment on the right eye. Computed tomography (CT) scans of the sinuses revealed a mucocele of the right frontal sinus with osteolysis and grade 2 exophthalmos, as well as an extra-conical process of the right orbit with lysis of the anterior and posterior walls of the right frontal sinus and the anterior and posterior ethmoidal cells. This required remote expertise from an ophthalmologist specialized in orbital diseases and a neuroradiologist to confirm the diagnosis of mucocele. Surgical treatment using the fronto-eyebrow approach of Jacques was performed and the post-operative outcome was satisfying six months later.
Conclusion: Fronto-ethmoid-orbital mucocele is a rare condition in our settings. Multidisciplinary expertise and remote expertise can be of great value in the diagnosis and choice of treatment in an environment with limited resources.
Keywords: Complications, Fronto-ethmoido-orbital mucocele, Management, Multidisciplinary expertise
Introduction
A nasal sinus mucocele is a benign cystic tumor that develops at the expense of the sinus mucous membranes and is due to a lack of ventilation of the sinus concerned [1]. Frequent localizations are frontal or fronto-ethmoid in 60% of cases [2]. Despite its histological benignity, this tumor has an aggressive potential in the orbit and brain that can lead to formidable complications [3],[4]. This lytic potential of the bone walls of the sinuses can sometimes pose diagnostic and management problems, thus requiring multidisciplinary expertise [5],[6]. The ENT and Ophthalmology Departments of Saint Joseph Hospital in Kinshasa, in collaboration with the team from the University of Rostock (ophthalmologist specialized in orbital diseases and neuroradiologist), took care of a case of giant fronto-ethmoido-orbital mucocele during the period from 22/11/2023 to 09/04/2024.
Objectives
The main objectives of this article were, on the one hand, to describe the clinical, radiological, and therapeutic characteristics of this condition and, on the other hand, to determine the place of telemedicine and multidisciplinary management in the event of complications of this condition in environments in resource-limited countries.
Case Report
A 38-year-old female patient, with no particular sinus history, referred to the Ophthalmology Department for better management of chronic sinusopathy complicated by documented mucocele. The early symptoms were marked (four years earlier) by redness and ocular globe protuberance of the right eye which were neglected. Two years later, during a pregnancy, the swelling worsened; this prompted the patient to consult an Ophthalmology Department.
The ENT examination on admission revealed exophthalmos with preservation of extrinsic oculomotor function. The rest of the ENT examination was unremarkable.
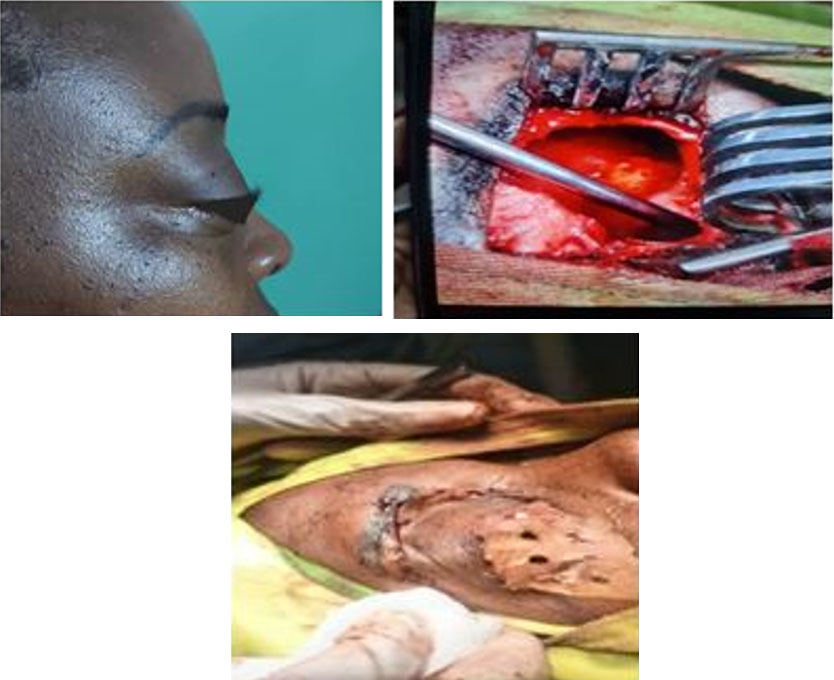
The ophthalmological examination already showed a visual impairment of 6/24 in the right eye and 6/9 in the left eye, a sensitivity to the pressure of the superior orbital rim in the supranasal of the right eye, axile exophthalmos with limitation of adduction and superduction, an intraocular pressure of 17.3 mmHg in the right eye and 14.6 mmHg in the left eye and diplopia (Figure 1).
The computed tomography (CT) scan of the sinus performed on 24/07/2023 concluded that there was chronic sinusopathy complicated by mucocele of the right frontal sinus and osteolysis with grade II exophthalmos (Figure 2A).
The sinus CT scan with contrast agent injection performed on 05/02/2024 suggested the presence of an extraconical tissue process of the right orbit responsible for grade 3 exophthalmos, the implantation base of which is located at the level of the inner wall. This mass was responsible for bone lysis extending to the level of the anterior and posterior ethmoid cells. It also extended to the right frontal sinus with lysis of the anterior wall (Figure 2B).
In view of this evolution of the lytic lesions on CT scans, the opinions of the ophthalmologist specialized in orbital diseases and the neuroradiologist was required by telemedicine. The specialists from the University of Rostock (Germany) consulted and confirmed the diagnosis of a right fronto-ethmoid mucocele in the first hypothesis, in view of the patient’s age and the bone which seemed to be enlarged rather than destroyed. Surgical drainage of sinus was advised.
The fronto-eyebrow approach of Jacques was then performed and showed a lysis of the anterior wall of the right frontal sinus causing a yellowish, sticky liquid to emerge, which had not been cultured. This fluid extended into the ethmoid cells with lysis of the orbital wall and the posterior wall of the sinus. A large fronto-ethmoidectomy allowed the complete excision of the cyst, the closure of the posterior wall of the right frontal sinus with bone wax, the repermeabilization and drainage of the nasofrontal canal thanks to a sloping drain left in place for two months
The postoperative effects were simple and the follow-up after six months was unremarkable. The ENT and ophthalmological examinations noted a very good evolution (visual acuity of 6/6, significant reduction in exophthalmos, absence of orbital rim pain, and disappearance of diplopia) both from a clinical and aesthetic point of view (Figure 3 and Figure 4).
Discussion
The objectives pursued by this article were first to describe the clinical, radiological, and therapeutic characteristics of this condition; secondly, to determine the place of telemedicine and multidisciplinary management in the event of complications of this condition in an environment with limited resources. From a clinical point of view, in our clinical case, the symptoms were dominated exophthalmos and diplopia, which led the patient to logically consult the ophthalmology department after four years of evolution without treatment. Indeed, it is described that the symptomatology of a fronto-ethmoid mucocele can remain silent for a long time, the initial signs are essentially dominated by frontal or orbital swelling, ocular signs as exophthalmos, diplopia, deviation of the eyeball with limitation of eye movements and in the late stage a decrease in visual acuity [7],[8].
From the point of view of diagnosis, the craniofacial CT scan is the examination of choice in case of clinical or endoscopic suspicion of mucocele and allows, apart from the diagnosis, to make an assessment of the bone lesions as described in the case under study. In case of diagnostic doubt, intraorbital or intracranial extension, magnetic resonance imaging (MRI) allows a better analysis of the lesions [3],[8],[9]. The latter was not carried out by the patient due to lack of financial means and we referred to the various expert advice for the choice of treatment. Indeed, the treatment of mucoceles is surgical: either externally (eyebrow or gingivo-jugal depending on the location) or endoscopic [4].
In the present clinical case, we opted for the external eyebrow route because of the diagnostic doubt, the description of bone lysis suggestive of an orbitoencephalic extension and anterior fistulization toward the soft tissues as well as the possibility of performing a large fronto-ethmoidectomy for a good drainage of the mucocele. The good clinical outcome after a 6-month follow-up justifies this choice and confirms the diagnosis of mucocele although bacteriological examinations of the secretions have not been carried out [10]. However, medium- and long-term monitoring is necessary to judge the success of the intervention (6–12 months) [11].
In addition, the management of our patient raises two problems: the first is related to the long evolution of the pathology before the actual treatment, and the second, raising the problem of managing the complications of this condition in environments with limited resources. This long standing of the pathology before the current treatment is the result of negligence and the lack of adequate resources in our environments, as demonstrated by the case in study.
In the series of Bouatay et al., the duration of evolution of the pathology was from 1 to 84 months, in particular because of the complex symptomatology: ophthalmological, neurological, rhinological, or aesthetic, demonstrating the major role of imaging in the diagnosis and management of mucoceles. Hence the interest of multidisciplinary care in the management of this condition [3].
This multidisciplinary management is becoming imperative, especially in the management of complications. Expansion toward the orbit and toward the brain represents the most severe complications of fronto-ethmoid mucoceles and requires the expertise of an ophthalmologist specialized in orbital diseases, a neurosurgeon or a neuroradiologist outside the ENT and the ophthalmologist. In environments where this expertise may be lacking, the use of a tele-expertise can give better quality of specialized care.
Conclusion
Fronto-ethmoidal mucocele is a rare condition in our environment. Its symptomatology is often silent for a long period of time, and this evolution can lead to bone lysis, which may extend to the orbit or brain. Craniofacial CT scan is the procedure of choice for diagnosis and magnetic resonance imaging provides a better analysis in cases of doubt. In resource-limited environments, multidisciplinary management including ophthalmologists, radiologists, neurologists, or even tele-expertise can lead to a judicious therapeutic choice.
REFERENCES
1.
2.
3.
Bouatay R, Aouf L, Hmida B, et al. The role of imaging in the management of sinonasal mucoceles. Pan Afr Med J 2019;34:3. [CrossRef]
[Pubmed]

4.
5.
6.
Lund VJ, Milroy CM. Fronto-ethmoidal mucocoeles: A histopathological analysis. J Laryngol Otol 1991;105(11):921–3. [CrossRef]
[Pubmed]

7.
8.
Bakhil A, Benbachir A, Buckat H, et al. Place de la voie crâniale dans la prise en charge des mucocèles frontales: A propos de deux cas et revue de littérature. IOSR Journal of Dental and Medical Sciences (IOSRJDMS) 2023;22(8):48–52. [CrossRef]

10.
11.
Facon F, Dessi P. Microinvasive endonasal surgery: Contribution of endoscopy to maxillofacial surgery. [Article in French]. Rev Stomatol Chir Maxillofac 2005;106(4):230–42. [CrossRef]
[Pubmed]

SUPPORTING INFORMATION
Author Contributions
Omadjela Oluku Augustin - Conception of the work, Design of the work, Acquisition of data, Analysis of data, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Kilangalanga Ngoy Janvier - Conception of the work, Design of the work, Acquisition of data, Analysis of data, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Lumbu Malundama Damien - Conception of the work, Design of the work, Acquisition of data, Analysis of data, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Yogolelo Asani - Analysis of data, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Atiko Nono Noel - Acquisition of data, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Geoffrey Rose - Conception of the work, Design of the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Guthoff Rudolf Friedrich - Conception of the work, Design of the work, Drafting the work, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Guaranter of SubmissionThe corresponding author is the guarantor of submission.
Source of SupportNone
Consent StatementWritten informed consent was obtained from the patient for publication of this article.
Data AvailabilityAll relevant data are within the paper and its Supporting Information files.
Conflict of InterestAuthors declare no conflict of interest.
Copyright© 2024 Omadjela Oluku Augustin et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information.